In it together – THH helps the community respond to COVID-19

Thorne Harbour Health was formed in 1983 as a central part of the Victorian community response to the HIV/AIDS epidemic. It provides a range of services which include prevention education, treatment and care of PLHIV and counselling services, as well as serving the health needs of lesbian, gay, bisexual, transgender, and intersex (LGBTI) communities.
What’s happening right now will, for many people, evoke memories of the “AIDS Crisis” (as it was first called) of the 1980s and 1990s. Then, as now, there was a lot of fear and confusion.
“There’s certainly similarities because HIV is probably the last major pandemic that we experienced in this country,” says Simon Ruth, CEO of Thorne Harbour Health (THH), “but there’s a lot of differences as well. HIV is a blood-borne virus, it’s not that easy to catch, it’s only spread through certain practices and it targeted marginalised people within the community.”
Although it didn’t seem so at the time, HIV actually spread relatively slowly. It took five years before a proper action plan was in place. Many lives were lost, many were disrupted, but it did not bring countries to a complete standstill.
COVID-19 is different.
“This is a disease that moves incredibly quickly,” says Ruth.
Where HIV introduced rules of engagement that, if followed, allowed things to go on as normal, COVID-19 has effectively vetoed any contact and expunged any semblance of normalcy.
“We have a dual function as an organisation: we’re an AIDS council, doing HIV prevention and supporting people who are living with HIV; and we’re an LGBTQI health organisation,” explains Ruth.
THH is a key contact point for a vulnerable segment of the community. It’s vital that they continue to operate but it means adapting to a whole new social paradigm.
“This is going to be an incredibly challenging time for everybody, around loneliness and boredom, and social isolation, and people are going to want to break the rules – and we’ve got to stick to it if we’re going to make this work,” says Ruth.
Counselling services are now being delivered via Skype, Facetime, and phone. They are putting as many resources as they can online and using Zoom to help manage remote staff.
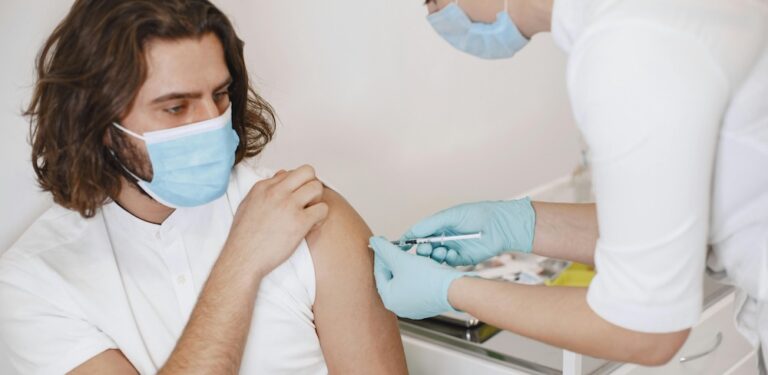
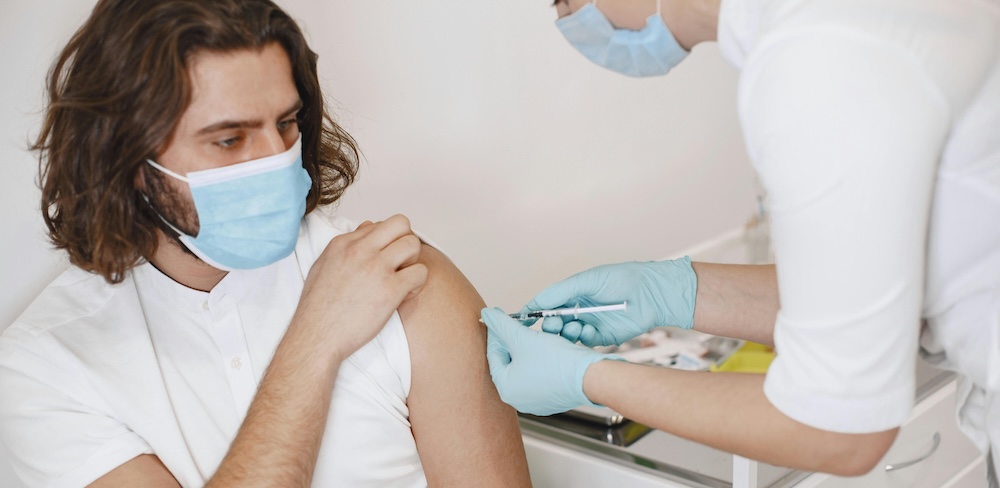
There are still some procedures such as hormone injections and flu shots that have to be administered in person. These will be by appointment only. HIV tests are currently only available at specific centres or online, but it’s hoped they may soon be made available at pharmacies. As for treatment, Ruth says there’s no need to worry.
“There’s nine drug companies that provide HIV medication to Australia and all nine have said there is no issue with supply of those drugs.”
Volunteers are helping fill the the service gaps, checking in on people who can no longer drop in to the Positive Living Centre, and providing much needed general support.
THH is working closely with other organisations such as Switchboard and Drummond Street in Victoria, and Shine in South Australia.